Free same day priority shipping
Buy quality peptides,
made in the USA
Leading the research industry
Showing 1–28 of 88 results
-

ACE-031 (1mg)
$161.00 -

Acetyl Hexapeptide-3 (Argireline) (200mg)
$210.00 -

Adipotide FTPP (10mg)
$77.00 -

AHK-Cu (200mg)
$192.00 -

AICAR (50mg)
$56.00 -

AOD 9604 (5mg)
$44.00 -

ARA-290 (16mg)
$88.00 -

B7-33 (6mg)
$62.00 -

BPC-157 (5mg & 10mg)
Price range: $52.00 through $92.00 -

BPC-157 & TB-500 & GHK-Cu Blend (70mg)
$305.00 -

BPC-157 & TB-500 Blend (10mg)
$115.00 -

Cardiogen (20mg)
$62.00 -

Chonluten (T-34) (20mg)
$62.00 -

CJC-1295 (Mod GRF 1-29) & Ipamorelin & GHRP-2 Blend (9mg)
$80.00 -

CJC-1295 & GHRP-2 Blend (10mg)
$84.00 -

CJC-1295 & GHRP-6 Blend (10mg)
$86.00 -
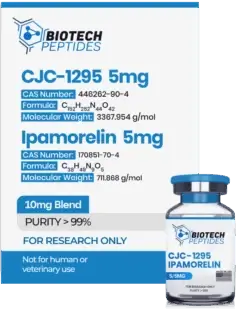
CJC-1295 & Ipamorelin Blend (10mg)
$81.00 -

CJC-1295 DAC (5mg)
$52.00 - Sale!

Decapeptide-12 (200mg)
Original price was: $239.00.$226.00Current price is: $226.00. -

DSIP (5mg)
$44.00 -

Epithalon (25mg)
$94.00 -

Follistatin-344 (1mg)
$162.00 -

FOXO4-DRI (Proxofim) (10mg)
$270.00 - Sale!

Fragment 176-191 (5mg)
Original price was: $47.00.$44.00Current price is: $44.00. -

Fragment 176-191 & CJC-1295 & Ipamorelin Blend (12mg)
$87.00 -

Fragment 176-191 & Mod GRF 1-29 & Ipamorelin Blend (12mg)
$87.00 -

GHK Basic (50mg)
$51.00 -

GHK Basic (Tripeptide-1) (200mg)
$165.00